
Welcome back to Life as a Cancer Survivor. Jelena here, and today I’m gonna talk about my treatment plan. This video and the last one kind of overlap with each other a bit, but if I would have combined them into one it would have been way too long so, you’re welcome. Here’s two medium length videos instead of one super long one. First things first, exactly what kind of cancer I had would determine what my treatment plan would be, so if you’re just getting started with this cancer rollercoaster, your treatment plan may differ some from mine because it depends on what type of colorectal cancer you have and what stage it is.
Let me know in the poll below if you or a loved one has been diagnosed with cancer, what stage was it? Was it stage 1, 2, 3, 4, or I’ll even put an option for you of I don’t know because maybe you’ve got a loved one and they don’t want to disclose all that information to you. I’d love to find out what stages everyone is in.
In my last video I talked all about the tests that I went through to get to this point, so if you missed that video, oh hey, here it is. Click on that link so you can watch that and figure out what kind of tests help with the staging to figure out how advanced your cancer is. At my first appointment with my oncologist on June 2nd, he only had the data from my colonoscopy and CT scan. He explained that colorectal cancer is staged by looking at three different things. T is the depth of the tumor invasion in your colon or your rectum. N is the number of lymph nodes that are involved. M is metastasis if it’s spread to any other organs in your body besides the one of your initial diagnosis.
He said he thought it looked like I was T3 N0 M0 which just means the level of the tumor was at a 3 and that it hadn’t spread to lymph nodes or other organs. But he said that in a CT scan it’s really hard to see if any lymph nodes near the rectum are involved, so hence the need for me to be referred to that rectal ultrasound. That rectal ultrasound would determine if any of those nearby lymph nodes were involved and it would also give us a more accurate rating of the tumor if it was anywhere from T1 to T3. He also said that there was a spot that showed up on my CT scan which was an enlarged lymph node that was near my heart, but he said it was unlikely that it would have been cancerous because if it was all the lymph nodes heading up to that one should have been infected as well. To be sure it wasn’t anything that we needed to be concerned about he sent me in for the PET scan.
 The PET scan would show that indeed the lymph node, the enlarged lymph node, in my chest was not cancer but there were multiple lymph nodes involved near the rectum. Ultimately he said that his prognosis for me was that this was curable and that my worst-case scenario would be that I would have a colostomy bag for the rest of my life. Hearing the oncologist say that he believed this was curable was a huge weight lifted off of my shoulders knowing that I was gonna survive this. Curable is not a term that oncologists throw around lightly so I knew that he was confident we were gonna get rid of this nasty cancer.
The PET scan would show that indeed the lymph node, the enlarged lymph node, in my chest was not cancer but there were multiple lymph nodes involved near the rectum. Ultimately he said that his prognosis for me was that this was curable and that my worst-case scenario would be that I would have a colostomy bag for the rest of my life. Hearing the oncologist say that he believed this was curable was a huge weight lifted off of my shoulders knowing that I was gonna survive this. Curable is not a term that oncologists throw around lightly so I knew that he was confident we were gonna get rid of this nasty cancer.
He said that if the tumor ended up being a T1 or a T2 they would just do surgery to get rid of it and that would be the end of my treatment. But if the tumor was rated T3 I would then have to do radiation and chemotherapy, then I would have surgery to remove the tumor, then perhaps adjuvant chemotherapy, which just means chemotherapy after your initial treatment has finished. My oncologist also noted that if I did have to do radiation and chemotherapy that it would be a low dose version of the chemo so there would be minimal side effects supposedly and I definitely wouldn’t lose my hair it just might thin. But also treatment would probably start in the next week or two.
The next day I had the rectal EUS, and at that appointment I found out that the tumor was rated a T3, and that nearby lymph nodes were also involved so that officially bumped me up to being diagnosed as Stage 3 Rectal Cancer. We also found out at that appointment that the tumor was only four centimeters away from my anal verge so my response to radiation would definitely determine whether or not I would end up with a permanent colostomy or just a temporary ileostomy. Four days later my oncologist confirmed with me the test results and what my treatment plan would be.
Step 1 of my treatment would be 25 days (actually 28) of radiation 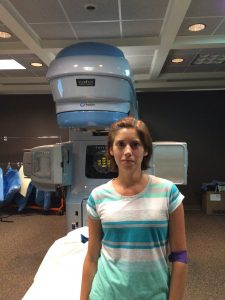 therapy and oral chemotherapy. I would go in five days a week for five and a half weeks for pelvic and on those days that I went in for radiation I would also take chemotherapy pills called Xeloda, also known as capecitabine I’m sure I’m pronouncing it wrong but Xeloda is much easier to pronounce and what everyone knows it as. I would take two pills in the morning within about a half-hour of eating and then about twelve hours later I would take three pills in the evening. I was also given a prescription for anti-nausea medication to have on hand in case I got nauseous from the chemotherapy pills. This part of my treatment would start on June 13, 2016.
therapy and oral chemotherapy. I would go in five days a week for five and a half weeks for pelvic and on those days that I went in for radiation I would also take chemotherapy pills called Xeloda, also known as capecitabine I’m sure I’m pronouncing it wrong but Xeloda is much easier to pronounce and what everyone knows it as. I would take two pills in the morning within about a half-hour of eating and then about twelve hours later I would take three pills in the evening. I was also given a prescription for anti-nausea medication to have on hand in case I got nauseous from the chemotherapy pills. This part of my treatment would start on June 13, 2016.
 Step 2 of my treatment would be major surgery. The doctor that would be doing my surgery preferred to wait 12 weeks after finishing radiation and chemotherapy to do the surgery. He liked to wait that long because after you’re done with those the tumor continues to shrink afterwards. During that surgery, the plan was to remove enough of my colon and rectum that there were clear margins that had no cancer cells in them on either side of the tumor. They would also remove an unknown number of lymph nodes, whatever looked like they were still cancerous that were nearby the rectum. Depending on how much my tumor shrank from step 1 would determine whether or not the tumor was far enough away to save my sphincter muscles and allow me to just have a temporary ileostomy or if they would have to take all of it and I would end up with a permanent colostomy.
Step 2 of my treatment would be major surgery. The doctor that would be doing my surgery preferred to wait 12 weeks after finishing radiation and chemotherapy to do the surgery. He liked to wait that long because after you’re done with those the tumor continues to shrink afterwards. During that surgery, the plan was to remove enough of my colon and rectum that there were clear margins that had no cancer cells in them on either side of the tumor. They would also remove an unknown number of lymph nodes, whatever looked like they were still cancerous that were nearby the rectum. Depending on how much my tumor shrank from step 1 would determine whether or not the tumor was far enough away to save my sphincter muscles and allow me to just have a temporary ileostomy or if they would have to take all of it and I would end up with a permanent colostomy.
A colostomy is where they run part of your large intestine out of your abdominal wall and then you wear a special bag over it to collect the waste that comes out of it. But if the tumor shrank well in step 1 and they were able to remove the tumor and preserve my sphincter muscles, well when they sew those two bits back together it’s called a resection. And when they resect those areas the chances of that connection site leaking are about 25%. So in order to prevent poop from leaking out of that connection site and swirling around in my stomach, they would do a temporary ileostomy which is where the small intestine is run out of your abdominal wall and you also wear a special bag over it to collect your waste that’s coming out of it. I’ll talk more about ostomies in a future video and I’ll explain them a little more in-depth, show you what mine looked like, and show you what some of the supplies are that you’d need if you have one.
Step 3 would happen depending on what they found inside of me during surgery but was most likely gonna happen just because of my age. Step 3 would take place six to eight weeks after surgery to give my body time to recover from all that slicing and dicing and it would be eight cycles of intravenous chemotherapy called FOLFOX. They wanted to do the second round for what they called mop-up chemo. Since I was so young at diagnosis and the cancer had spread to my lymph nodes they weren’t sure if any stray cells had gotten loose and were swirling around in my lymphatic system just waiting to multiply and spread more. So to make extra sure that they killed all the cancer cells and would give me tons of cancer-free years after this they voted to go aggressive with my treatment and have me do eight cycles of chemotherapy after surgery.
surgery but was most likely gonna happen just because of my age. Step 3 would take place six to eight weeks after surgery to give my body time to recover from all that slicing and dicing and it would be eight cycles of intravenous chemotherapy called FOLFOX. They wanted to do the second round for what they called mop-up chemo. Since I was so young at diagnosis and the cancer had spread to my lymph nodes they weren’t sure if any stray cells had gotten loose and were swirling around in my lymphatic system just waiting to multiply and spread more. So to make extra sure that they killed all the cancer cells and would give me tons of cancer-free years after this they voted to go aggressive with my treatment and have me do eight cycles of chemotherapy after surgery.
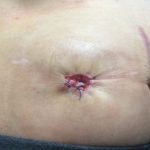 Step 4 would happen one to two months after my final cycle of chemotherapy if I ended up with a temporary ileostomy. I would have those 1-2 months to recover from those cycles of chemotherapy, build up my strength, build up my immune system, and they would reverse that ileostomy.
Step 4 would happen one to two months after my final cycle of chemotherapy if I ended up with a temporary ileostomy. I would have those 1-2 months to recover from those cycles of chemotherapy, build up my strength, build up my immune system, and they would reverse that ileostomy.
And that was the plan. It was all gonna take place over the course of just one year, but it was gonna be a long year. I just had to plug through each step one at a time to get to the finish line. One thing I’ve learned from all of these appointments is it’s really important to bring a friend or family member with you to them. That second set of ears really picks up extra little things here and there that you don’t. And also make sure you’re taking notes. Pen and paper, phone, computer, whatever your method of taking notes is do it because you’ll forget at least half of this stuff by the time you leave the doctor’s offices.
Tune in next week to hear how we decided to break the news to our five-year-old daughter Maelle, and her reaction to hearing that I might have some nighttime diarrhea during treatment. If you like this video, please hit the thumbs up button over here and make sure you’re subscribed so you’re the first to know what all of my new videos are posted. And if you have any friends that you think might be interested in some of these please feel free to share them that’s what I’m here for! Thank you for watching!
*This video was originally published on November 6, 2019
2 thoughts on “The Treatment Plan”